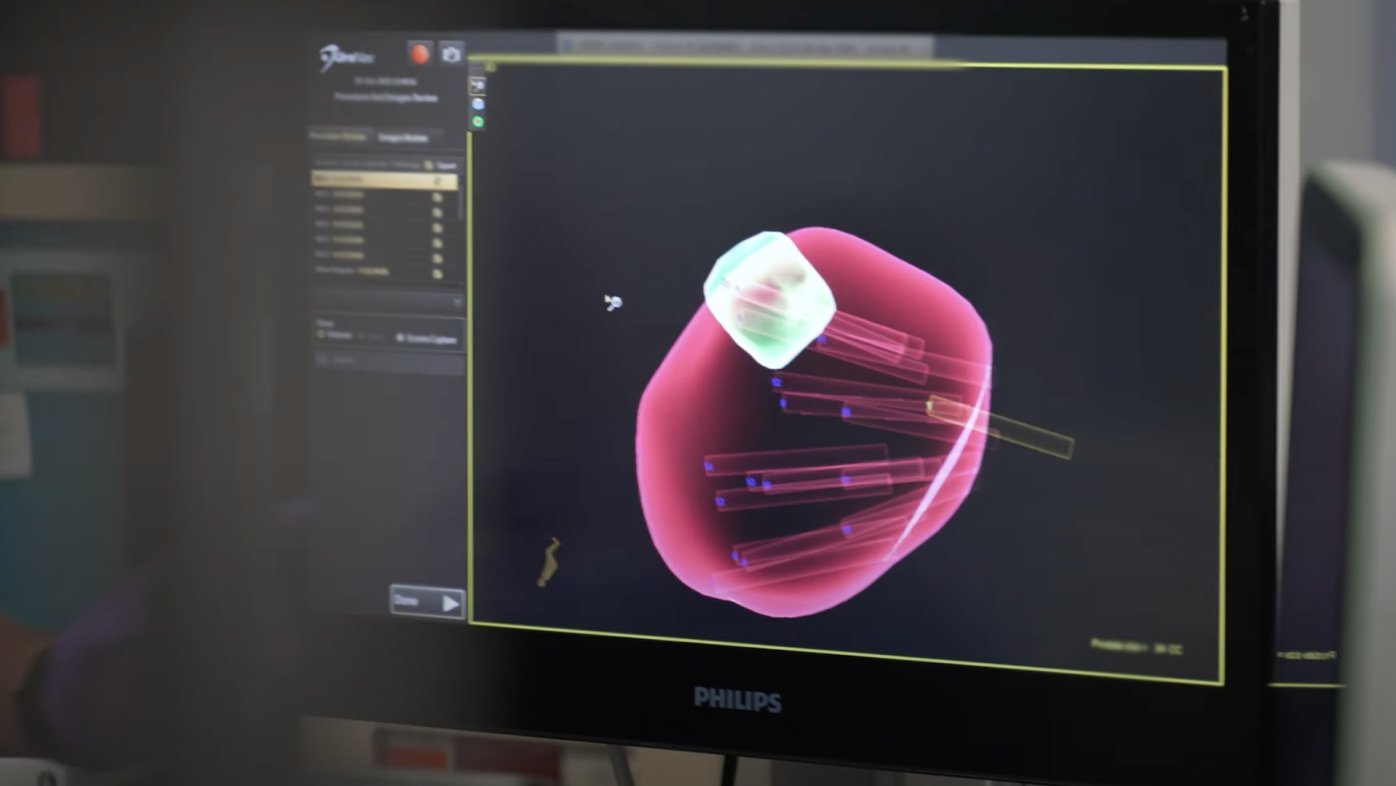
MRI guided prostate biopsy: A more accurate tool (video)
MRI guided prostate biopsy can provide a more accurate prostate cancer diagnosis to determine whether active surveillance or curative treatment is appropriate.
Lupus is a chronic autoimmune disease that affects several areas of your body, including your joints, skin, blood vessels and several major organs. It causes your immune system to produce antibodies that attack healthy organs and tissues within your body rather than foreign substances, such as bacteria and viruses, as it should.
Along with being difficult to diagnose and dangerous if left untreated, lupus is hard to endure and often misunderstood by non-sufferers.
Here are five facts about lupus that those affected would like you to know:
Lupus is unpredictable with symptoms that greatly vary. Sufferers experience pain and swelling in their joints and muscles, fever, rashes, chest pain, hair loss, ulcers in the mouth, swelling in the legs and face and swollen glands. Many feel very tired when experiencing these symptoms, called flares, which can come and go, and vary from mild to life-threatening.
Anyone can get lupus. More than 1.5 million Americans have lupus. While it affects mostly women between ages 15 to 44, men and children can get it, too. Women of African-American, Hispanic, Asian and Native American descent are two to three times more likely to develop the disease.
Lupus is not contagious. You cannot “catch” lupus from someone through any kind of contact and lupus cannot be sexually transmitted. It is also not a form of cancer; though, like cancer, extreme cases can be treated with chemotherapy.
Lupus is treated by a variety of doctors. A lupus patient’s health care team might consist of a family doctor, rheumatologist (doctor that treats arthritis and joint conditions), immunologist (immune system specialist), nephrologist (kidney specialist), hematologist (blood specialist), dermatologist (skin specialist) neurologist (nervous system specialist), cardiologist (heart specialist), endocrinologist (hormones specialist), psychologist and others.
Lupus affects the body and mind. Coping with lupus can be very stressful, creating a vicious cycle because stress can contribute to flares. Sufferers report feelings of isolation and depression because of the toll fatigue takes on their professional and social lives. Patients should surround themselves with a good support system including friends, family, support groups and their health care team; exercise regularly; and educate themselves to recognize the warning signs of flares, such as fatigue and achiness.
“Left untreated, active lupus may result in a number of complications, including various symptoms of illness as well as internal organ injury or failure,” says Dr. Dean Mayer, a rheumatologist with Sharp Rees-Stealy Medical Group. “However, there is effective treatment with medication, which is the best strategy to reduce flares. Patients should talk with their physician about developing an appropriate plan to address their individual needs.”
Our weekly email brings you the latest health tips, recipes and stories.