
Why does my knee hurt?
Learn more about three common causes of knee pain, and what to do to find relief.

A team of medical professionals from the U.S., including nurses from Sharp Chula Vista Medical Center, worked with hospital teams in Mexico to identify ways to improve patient care for those with COVID-19.
Lying on one's back places compressive pressure on the heart and lungs, which is especially dangerous for patients with
COVID-19, who can experience acute respiratory distress and require ventilation.
"Proning," or placing patients face down to reduce pressure on the chest cavity, allows for better oxygenation of the lungs and removal of pulmonary secretions - crucial milestones for removing a ventilator and allowing a patient to breathe on their own.
While proning has long been a best practice for patients in respiratory distress, the practice typically involves a mechanical bed to turn patients safely. When the number of Sharp hospital patients who needed proning exceeded the number of RotoProne beds, a team of nurse educators looked to the past for the answer.
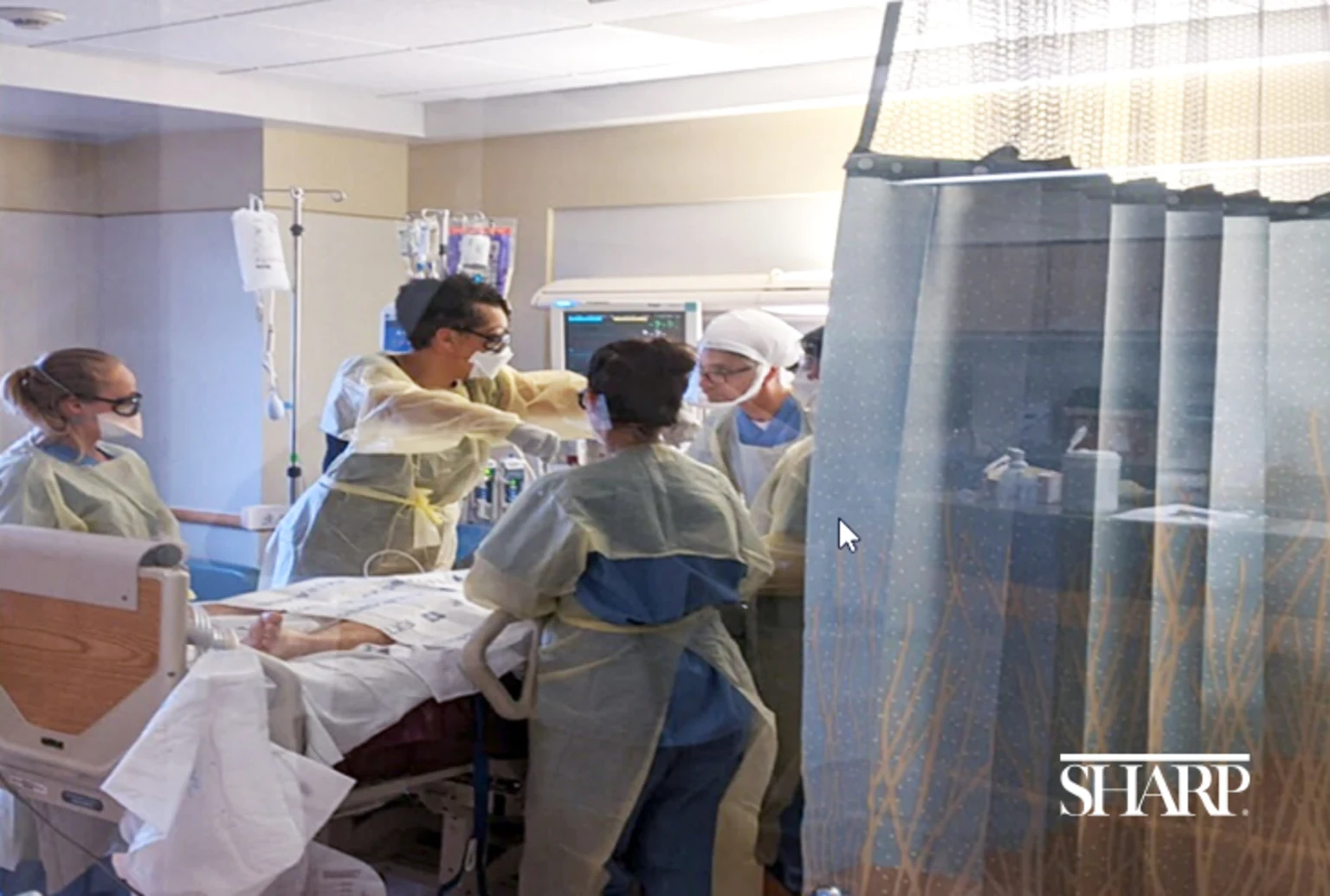
A team in the medical intensive care unit (MICU) at Sharp Chula Vista Medical Center practices the manual patient proning procedure.
"We discovered early that we would not have enough beds, so we looked at literature," says Christina Kelley, DNP, RN, a clinical nurse specialist at
Sharp Chula Vista Medical Center. "Thirty years ago, they didn't have RotoProne beds, so how did they do it? There was a methodical approach using human muscle to pronate a patient with a set of sheets."
Sharing best practices with hard-hit hospitals in Mexico
With the practice established in San Diego County, Kelley and a colleague reached out to hospitals in Tijuana and Mexicali, Mexico, and offered to teach the simplified manual technique to caregivers there. Few hospitals along the U.S.-Mexico border have a substantial supply of mechanical beds and many have been overwhelmed with patients with COVID-19 who require the use of ventilators.
"COVID-19 is the same everywhere, so if our patients are experiencing this, theirs are too," says Kelley. "We were able to share our best practices to speed them along. In Mexicali, the proning procedure derived from teaching hospitals in Mexico City was very lengthy and comprehensive, so we lined it up with ours, which is a simplified version that works better in clinical settings, to create a teaching and stepwise process for patient rooms, to allow manual proning to be done right every time."
Teams of nurse educators from Sharp Chula Vista have visited hospitals in Mexico to assess needs and identify best practices that could be adapted there. Teams then visit for physically distanced teaching sessions and follow-up assessments.
"The goal is to walk alongside nurses in Mexico, not to take over, but be there in consultation manner, as another set of eyes," says Kelley. "In this setting you can develop tunnel vision, so having a fresh set of eyes can help. We can say, 'have you tried this?'"
Other shared best practices include good oral hygiene for patients on ventilators, the use of proning for patients who are not yet in acute respiratory distress, and sedation stewardship - preventing adverse outcomes from deep sedation of intubated patients.
While the mortality rate for patients with COVID-19 along the border remains high, Kelley and her colleagues are encouraged by reports that the hospitals with which they have worked have been able to remove patients from ventilators.
In addition to its use as a technique for patients with COVID-19, the revised manual proning protocol is being reviewed for use during flu season, when demand for RotoProne beds is high.
For the news media: To talk with Christina Kelley about Sharp's work in Mexico for an upcoming story, contact Erica Carlson, senior public relations specialist, at
erica.carlson@sharp.com.
The Sharp Health News Team are content authors who write and produce stories about Sharp HealthCare and its hospitals, clinics, medical groups and health plan.

Christina Kelley, DNP, RN, is a clinical nurse specialist at Sharp Chula Vista Medical Center.

Our weekly email brings you the latest health tips, recipes and stories.