
Patient navigator brings comfort and clarity to care
As a patient navigator at Sharp Chula Vista, Jorge Martinez helps patients and loved ones feel more at ease during emergency room visits.
Dr. Nick Saade has seen a lot. An emergency medicine doctor affiliated with Sharp Memorial Hospital, he treats a wide variety of ailments and injuries every day as patients come through the Emergency Department. But nothing could have prepared him for the challenge of seeing his wife become a patient — while pregnant with their first child.
“We went through things I had little or no experience with,” says Dr. Saade. “Fortunately, we had an incredible team at Sharp Mary Birch Hospital for Women & Newborns to guide us.”
The early warning signs
The baby was due in early February 2026. However, around midway through her second trimester, Dr. Saade’s wife, Arriel, developed high blood pressure. By October, Arriel was being monitored for preeclampsia by her OBGYN, Dr. Sara Junya.
Preeclampsia is a condition where a pregnant mother’s blood pressure becomes elevated after the 20th week of pregnancy. The high blood pressure can sometimes impact other organs, such as the liver or kidneys. It occurs in nearly 10% of pregnancies.
“We don’t know exactly what causes preeclampsia,” says Dr. Junya. “Sometimes there are no symptoms, other than high blood pressure. Other times, patients experience symptoms such as headaches, spots in vision, chest pressure, or pain under the right side of the ribs.”
Risk factors associated with preeclampsia include:
Age of the pregnant mother
First pregnancies
Obesity
Family history of preeclampsia on either the mother’s or father’s side
“During pregnancy, there are always surprises and choices,” says Dr. Junya. “With preeclampsia, I try to prepare my patients for all the possibilities without overwhelming them. That includes knowing one of those possibilities is that there may come a time when it’s too risky to continue with the baby in utero.”
Arriel and Dr. Saade made sure to complete their baby preparations several weeks before the due date — just in case their baby needed to be delivered early.
Decision time
Arriel began experiencing common preeclampsia symptoms, including headaches, spots in her vision and abdominal pain. On Dec. 17, those symptoms intensified. Dr. Saade drove her to Sharp Mary Birch.
Arriel’s blood pressure was high, and she was admitted as a precaution. A specialist in high-risk pregnancies was brought in to examine her. The specialist and Dr. Junya agreed that the risk to Arriel’s health was increasing and that the family should consider delivering the baby early. When lab tests raised concerns, Arriel and Dr. Saade decided to move forward with a cesarean section delivery that evening.
“This is where the science of medicine becomes an art,” explains Dr. Junya. “The baby is really the one in charge. He was telling us it was time to be born.”
Into the NICU
Leo Saade was delivered weighing a solid 5 pounds, 5 ounces — despite being born seven weeks prematurely — then taken to the Neonatal Intensive Care Unit (NICU). Despite all Dr. Saade had seen in his career, the sight of his baby son hooked up to an oxygen machine sent him to the verge of tears.
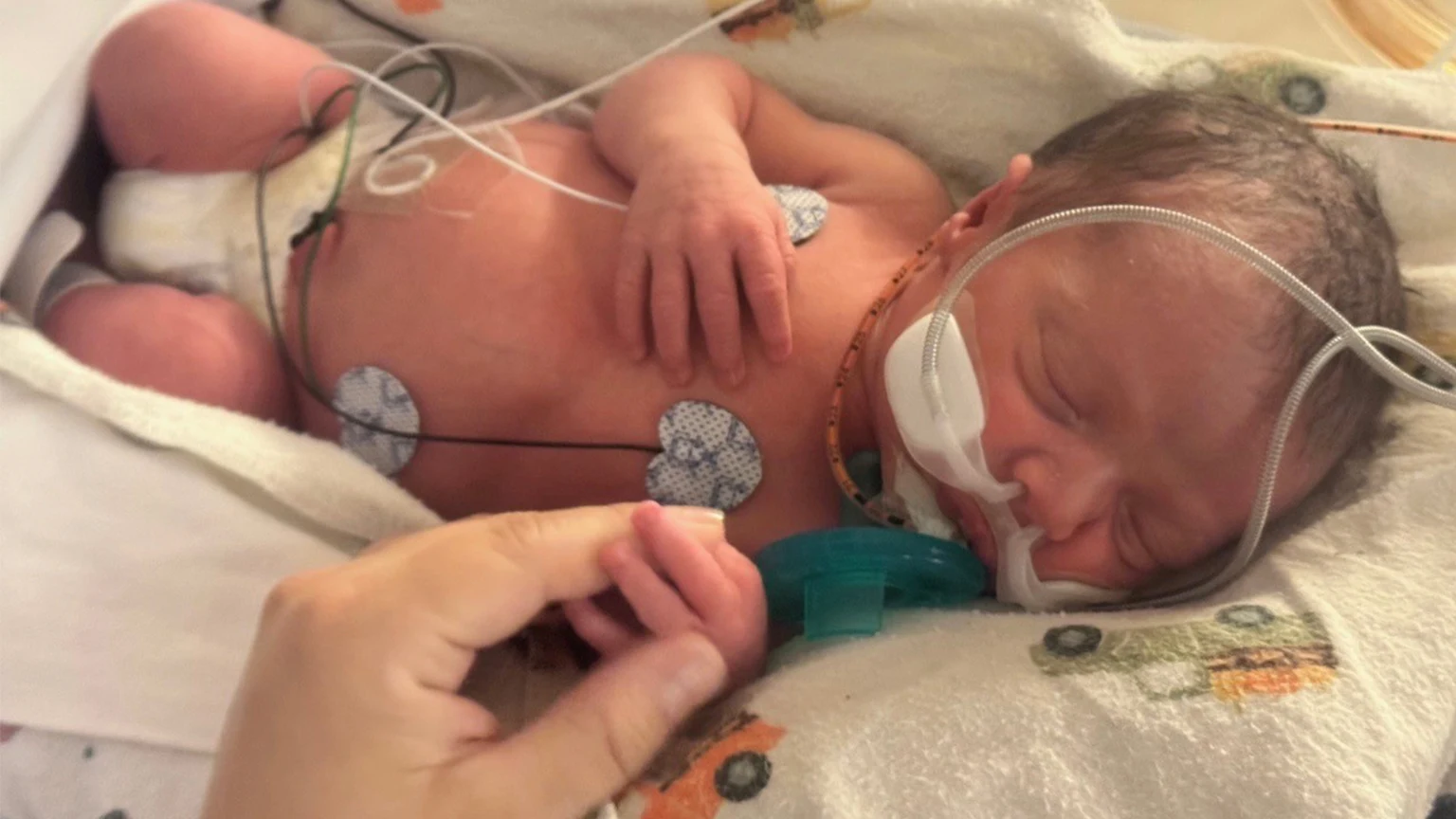
Baby Leo Saade in the NICU at Sharp Mary Birch Hospital for Women & Newborns.
“It was scary. But because I’m a doctor, I have a sixth sense about when things are going wrong, and I wasn’t getting any of those signals from the team in the NICU. I began to realize that they weren’t worried, so I didn’t need to be. They explained what was happening and that it was very routine.
“This was the field of medicine I had the least amount of experience with. I was in awe of how great the Sharp Mary Birch team is.”
While Leo was treated in the NICU, Dr. Junya was taking care of Arriel. “Mothers can still have preeclampsia up to six weeks after delivery, and the first 24 hours are critical. Blood pressure can change quickly, and preeclampsia can develop into eclampsia, which is life-threatening and can include seizures and stroke,” says Dr. Junya.
Out of the NICU
Fortunately, Arriel recovered well, as did Leo. Arriel remained in the hospital for five days after the delivery before returning home. The original estimate was that Leo may need to stay in the NICU for a month, but he gained strength so quickly that he was able to go home after just two weeks. Because Arriel and Dr. Saade had prepared for the possibility of an early birth, their home was ready to welcome them back as an expanded family of three.
“It’s a privilege to help every family welcome new life into the world,” Dr. Junya says. “But to have a Sharp colleague like Dr. Saade put the health of his wife and baby under my care is very humbling and a true honor.”
“It wasn’t easy to see my wife and baby become patients,” Dr. Saade reflects. “But seeing the care and professionalism of the team at Sharp Mary Birch will help me become a better doctor with my own patients.”

Dr. Nick Saade smiles at his new baby, Leo, at Sharp Mary Birch Hospital for Women & Newborns.
Learn more about pregnancy; get the latest health and wellness news, trends and patient stories from Sharp Health News; and subscribe to our weekly newsletter by clicking the "Sign up" link below.

Our weekly email brings you the latest health tips, recipes and stories.